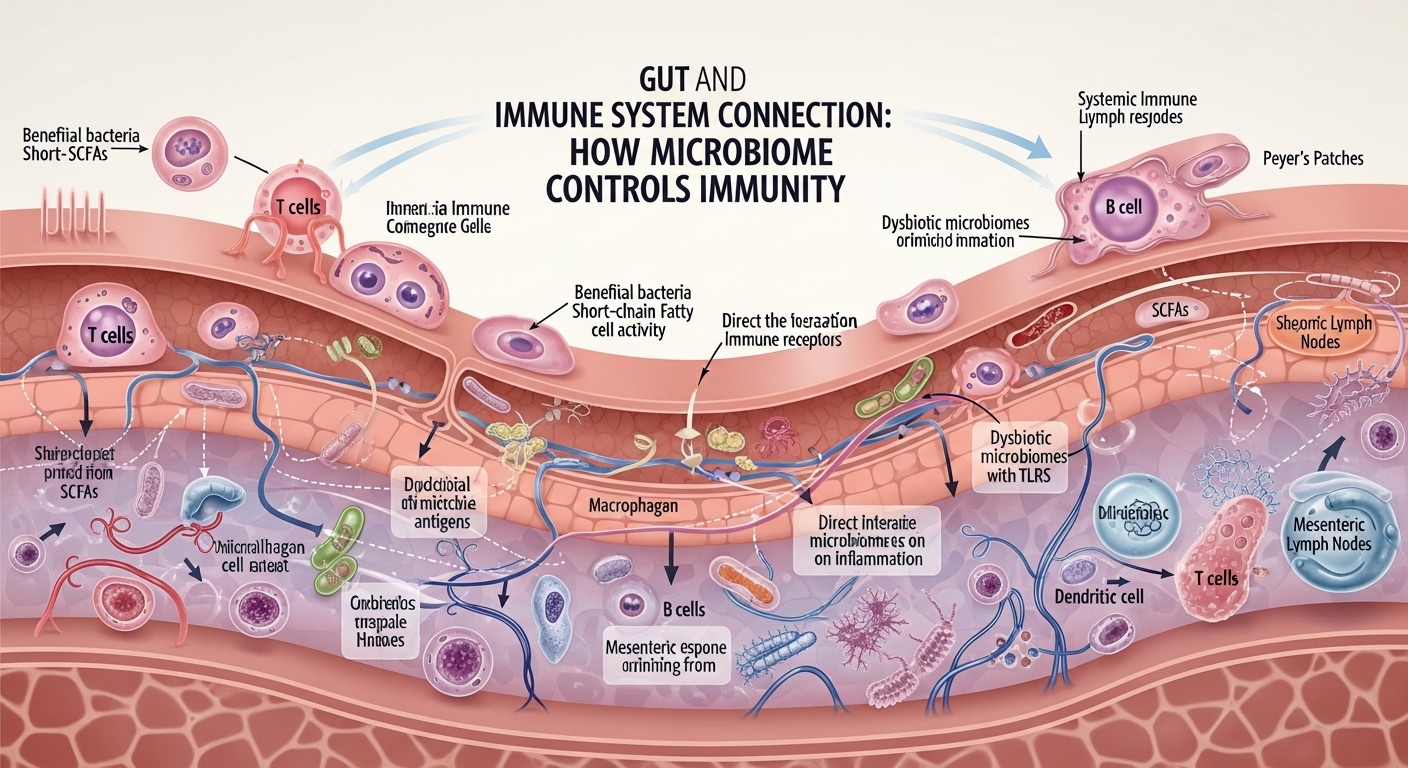
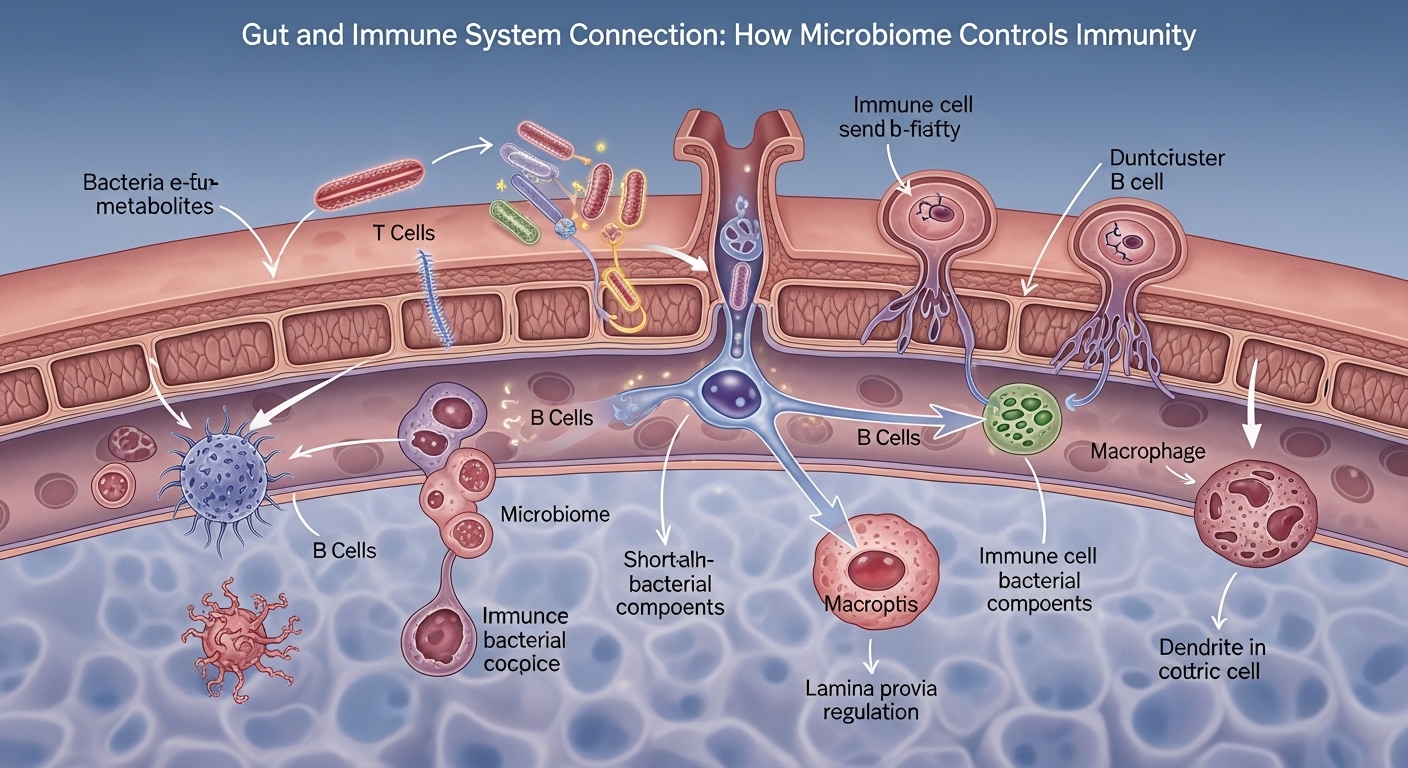
Your immune system does not begin in your bloodstream. It begins in your gut. Nearly 70% of immune cells live inside your digestive tract, interacting with trillions of microbes that decide whether your body fights disease efficiently or stays stuck in inflammation.
Many people try supplements, detox plans, or strict diets without realizing their gut bacteria already control immune performance. When the microbiome becomes unbalanced, infections increase, allergies worsen, and recovery slows.
The good news is this system responds quickly to simple daily habits. Once you understand how the gut regulates immunity, you can strengthen your defenses naturally and consistently.
How Does the Gut Control the Immune System?
Snippet Answer (50 words): The gut controls the immune system by hosting most immune cells and regulating how they respond to threats. Beneficial bacteria train immune cells, reduce inflammation, strengthen the intestinal barrier, and prevent pathogens from entering the bloodstream. A balanced microbiome supports faster responses and stronger long-term protection against disease.
Answer Block (48 words): The gut controls immunity by acting as the training center for immune cells. Microbes communicate with immune tissues, regulate inflammation levels, and block harmful organisms from entering circulation. A healthy microbiome improves immune accuracy, while imbalance increases infection risk and chronic inflammatory disease.
Your digestive tract contains the gut-associated lymphoid tissue (GALT). This network detects threats and decides whether to activate immune defenses or tolerate harmless substances like food proteins.
Beneficial bacteria produce short-chain fatty acids such as butyrate. These molecules strengthen intestinal cells and prevent toxins from leaking into the bloodstream.
When this protective barrier weakens, immune cells overreact. That overreaction increases allergies, autoimmune symptoms, and fatigue.
A strong microbiome improves:
- Immune cell communication
- Antibody production
- Inflammation control
- Pathogen detection speed
This explains why gut health influences nearly every immune-related condition.
Why Are 70% of Immune Cells Located in the Gut?
Answer Block (46 words): About 70% of immune cells live in the gut because it is the body’s main entry point for microbes and foreign particles. Immune tissues there constantly monitor threats from food, bacteria, and toxins, allowing early detection and prevention before infections spread.
Your digestive tract interacts with the outside world more than any other organ system. Every meal introduces bacteria, viruses, and environmental chemicals.
Because of this exposure, the immune system concentrates surveillance inside intestinal walls.
Specialized immune structures inside the gut include:
- Peyer’s patches that detect pathogens
- Dendritic cells that present antigens
- Secretory IgA antibodies that neutralize microbes
- Regulatory T cells that prevent immune overreaction
These systems create balance between defense and tolerance. Without them, the immune system would attack harmless substances constantly.
Efficient immune training inside the gut explains why microbiome disruption weakens resistance across the entire body.
What Happens When Gut Bacteria Become Imbalanced?
Answer Block (47 words): When gut bacteria become imbalanced, harmful microbes increase inflammation and weaken immune signaling. This condition, called dysbiosis, damages the intestinal barrier and allows toxins into circulation. The immune system then becomes overactive or ineffective, increasing infections, allergies, and autoimmune risk.
Dysbiosis develops slowly but affects immunity quickly.
Common triggers include:
- Low-fiber diets
- Frequent antibiotic use
- Chronic stress
- Sleep disruption
- Ultra-processed foods
Once beneficial bacteria decline, inflammatory microbes expand. These organisms produce endotoxins that activate immune alarms unnecessarily.
The result is persistent low-grade inflammation. Over time, this contributes to:
- Digestive disorders
- Skin problems
- Frequent infections
- Brain fog
- Metabolic imbalance
Restoring microbial diversity often improves symptoms faster than expected.
How Does the Gut Barrier Protect Against Disease?
Answer Block (45 words): The gut barrier protects immunity by preventing harmful microbes and toxins from entering the bloodstream. Tight junction proteins seal intestinal cells together while beneficial bacteria reinforce this barrier. When intact, the barrier reduces inflammation and infection risk across multiple organ systems.
The intestinal lining acts like a selective filter. Nutrients pass through. Harmful particles stay out.
This protection depends on tight junction proteins that connect intestinal cells closely together.
When inflammation weakens these connections, intestinal permeability increases. This condition is often called “leaky gut.”
Once permeability rises:
- Toxins enter circulation
- Immune cells activate unnecessarily
- Inflammation spreads systemically
- Energy levels decline
Beneficial bacteria restore barrier strength by producing protective metabolites and maintaining mucus layers.
This is one reason dietary fiber supports immunity so strongly.
Which Foods Strengthen the Gut–Immune Connection Most?
Answer Block (49 words): Foods that strengthen the gut–immune connection include fiber-rich plants, fermented foods, polyphenol-containing fruits, and omega-3 sources. These foods increase beneficial bacteria, reduce inflammation, and improve intestinal barrier integrity. Regular intake supports immune signaling and reduces infection frequency over time.
Diet shapes microbial diversity more than any supplement.
The most effective immune-supporting foods include:
- Vegetables like spinach, broccoli, and carrots
- Fermented foods like yogurt and kefir
- Legumes and whole grains
- Garlic and onions
- Green tea and berries
Fiber feeds beneficial microbes directly. Fermented foods introduce helpful bacteria. Polyphenols improve microbial balance.
Together, these nutrients create an anti-inflammatory intestinal environment that improves immune coordination.
| Food Type | Primary Benefit | Immune Impact |
|---|---|---|
| Fermented foods | Add beneficial bacteria | Improve antibody response |
| Fiber-rich vegetables | Feed microbiome | Reduce inflammation |
| Polyphenol fruits | Support microbial diversity | Strengthen immune signaling |
| Omega-3 sources | Lower inflammatory markers | Enhance immune balance |
Can Stress Damage the Gut and Weaken Immunity?
Answer Block (46 words): Stress weakens immunity by disrupting gut bacteria and increasing intestinal permeability. Stress hormones alter microbial composition and reduce protective species. Over time, this increases inflammation and lowers resistance to infections, making stress management essential for maintaining a strong gut-immune connection.
The gut and brain communicate continuously through the gut–brain axis.
During stress, cortisol levels increase. Elevated cortisol changes microbial balance and slows digestion.
These effects reduce beneficial bacteria and increase inflammatory species.
Chronic stress also:
- Weakens intestinal barrier function
- Reduces immune cell coordination
- Increases susceptibility to viruses
- Slows recovery after illness
Improving sleep, exercise consistency, and relaxation routines restores microbial stability surprisingly quickly.
How Long Does It Take to Improve Gut-Driven Immunity?
Answer Block (44 words): Gut-driven immunity can begin improving within days of dietary changes, but lasting benefits typically appear after several weeks. Consistent fiber intake, probiotic foods, sleep improvements, and stress reduction gradually restore microbial diversity and strengthen immune defenses over time.
The microbiome responds faster than most people expect.
Studies show measurable microbial changes within 48 hours of increasing plant diversity.
However, long-term immune improvements require consistent habits.
A realistic improvement timeline looks like this:
- Week 1: digestion stabilizes
- Week 2: inflammation begins decreasing
- Week 3–4: immune resilience improves
- Month 2+: infection resistance increases
Consistency matters more than intensity.
Do Probiotics Actually Improve Immune Function?
Answer Block (48 words): Probiotics can improve immune function by restoring beneficial bacteria that regulate inflammation and strengthen the intestinal barrier. They support antibody production and reduce infection duration, but their effectiveness depends on strain selection, diet quality, and consistency rather than short-term supplementation alone.
Not all probiotic strains provide the same benefits.
Evidence supports strains such as:
- Lactobacillus rhamnosus
- Bifidobacterium lactis
- Lactobacillus plantarum
These strains improve immune signaling and reduce respiratory infections.
However, probiotics work best when combined with fiber-rich foods that feed existing beneficial microbes.
Without dietary support, their effects remain temporary.
Conclusion: How Can You Strengthen Your Gut to Support Immunity?
Your immune system depends heavily on the condition of your microbiome. When gut bacteria remain balanced, immune cells respond faster and inflammation stays controlled. When imbalance develops, protection weakens across multiple systems.
The solution is practical and achievable.
Increase plant diversity. Eat fermented foods regularly. Sleep consistently. Reduce chronic stress. Limit ultra-processed foods.
These habits restore microbial stability and strengthen immune defenses naturally.
If you want fewer infections, faster recovery, and better long-term health, improving gut health is one of the most reliable strategies available today.
Start with one small change this week. Add one fiber-rich meal daily. That single step begins strengthening your immune system immediately.
FAQ: Gut Health and Immune System Connection
Can poor gut health cause frequent infections?
Yes. Poor gut health weakens immune signaling and reduces antibody production. This makes the body slower at detecting pathogens and increases infection frequency.
Does sugar harm gut bacteria?
High sugar intake feeds inflammatory microbes and reduces beneficial bacteria. Over time, this imbalance weakens immune coordination.
Is yogurt enough to improve gut immunity?
Yogurt helps but works best alongside fiber-rich vegetables, legumes, and whole grains that support long-term microbial diversity.
How does fiber strengthen immunity?
Fiber feeds beneficial microbes that produce anti-inflammatory compounds. These compounds reinforce the intestinal barrier and improve immune cell communication.
Can antibiotics permanently damage gut immunity?
Antibiotics temporarily reduce microbial diversity. Recovery usually occurs with fiber intake, fermented foods, and time.
Does sleep affect the gut microbiome?
Yes. Poor sleep disrupts microbial balance and increases inflammation, which weakens immune performance.
Are probiotics necessary for everyone?
No. Many people improve gut immunity through diet alone, but probiotics help during illness recovery or after antibiotic use.
Read More Also: Beginner’s Guide to Eyeliner: Tips for Perfecting Your Flick